 The study sample consisted of 3451 consecutive patients admitted to the University of Michigan between January 1999 and December 2005 with a discharge diagnosis of ACS. Moreover, we sought to investigate the relative contributions of model simplicity and model composition to any observed prognostic differences between the TIMI and GRACE risk scores. This study aimed to evaluate the prognostic abilities of the TIMI and GRACE risk scores over a broad-spectrum of community-derived ACS patients (UA/NSTEMI and STEMI) admitted to a tertiary care center. Comparisons of the TIMI and GRACE scores in STEMI patients remain unexplored. Recent studies have suggested the superiority of the GRACE risk scores as compared to the TIMI UA/NSTEMI score in UA and/or NSTEMI patients. Though slightly more complex, the GRACE risk scores for in-hospital and 6-month mortality are derived from a more representative community-based registry. The TIMI risk scores for Unstable Angina/Non ST-Elevation Myocardial Infarction (UA/NSTEMI) and for ST-Elevation Myocardial Infarction (STEMI) patients are simple, integer-based scores derived from selected clinical-trial cohorts. 
Both of these scoring systems have been shown to predict the response of ACS patients to various treatment modalities, and may therefore significantly influence therapeutic decision-making. Current AHA/ACC guidelines promote the use of the Thrombolysis in Myocardial Infarction (TIMI) and Global Registry of Acute Coronary Events (GRACE) risk scores to evaluate the in-hospital and post-discharge risk of ACS patients. Risk stratification is integral to the management of patients presenting with Acute Coronary Syndromes (ACS). The remaining authors report no conflicts. Gurm has received research support from Blue Cross Blue Shield Foundation of Michigan, and the NIH. Goodman has received research grant support and speaker/consulting honoraria from Sanofi-aventis, the sponsor for the ESSENCE and TIMI 11B trials, and the GRACE project. Eagle has received research support from the Mardigian Foundation, Sanofi-aventis, Pfizer, and the Department of Internal Medicine, University of Michigan. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.Ĭompeting interests: Dr. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.įunding: The present work was supported in part by unrestricted grants from: Sanofiaventis, Pfizer, the Blue Cross Blue Shield Foundation, the Mardigian Foundation, and the University of Michigan Health System. Received: SeptemAccepted: OctoPublished: November 23, 2009Ĭopyright: © 2009 Aragam et al. Hernandez, Lerner Research Institute, Cleveland Clinic, United States of America  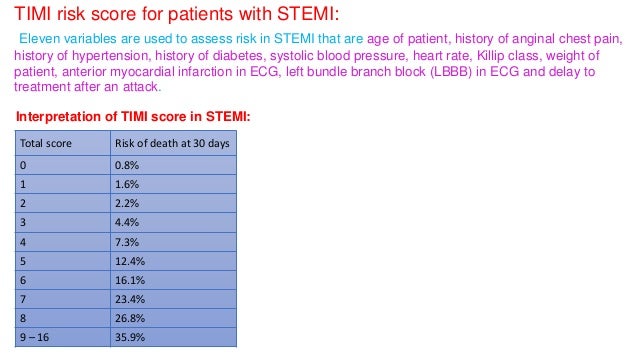
(2009) Does Simplicity Compromise Accuracy in ACS Risk Prediction? A Retrospective Analysis of the TIMI and GRACE Risk Scores. Study limitations included unaccounted for confounders inherent to observational, single institution studies with moderate sample sizes.Ĭitation: Aragam KG, Tamhane UU, Kline-Rogers E, Li J, Fox KAA, Goodman SG, et al. 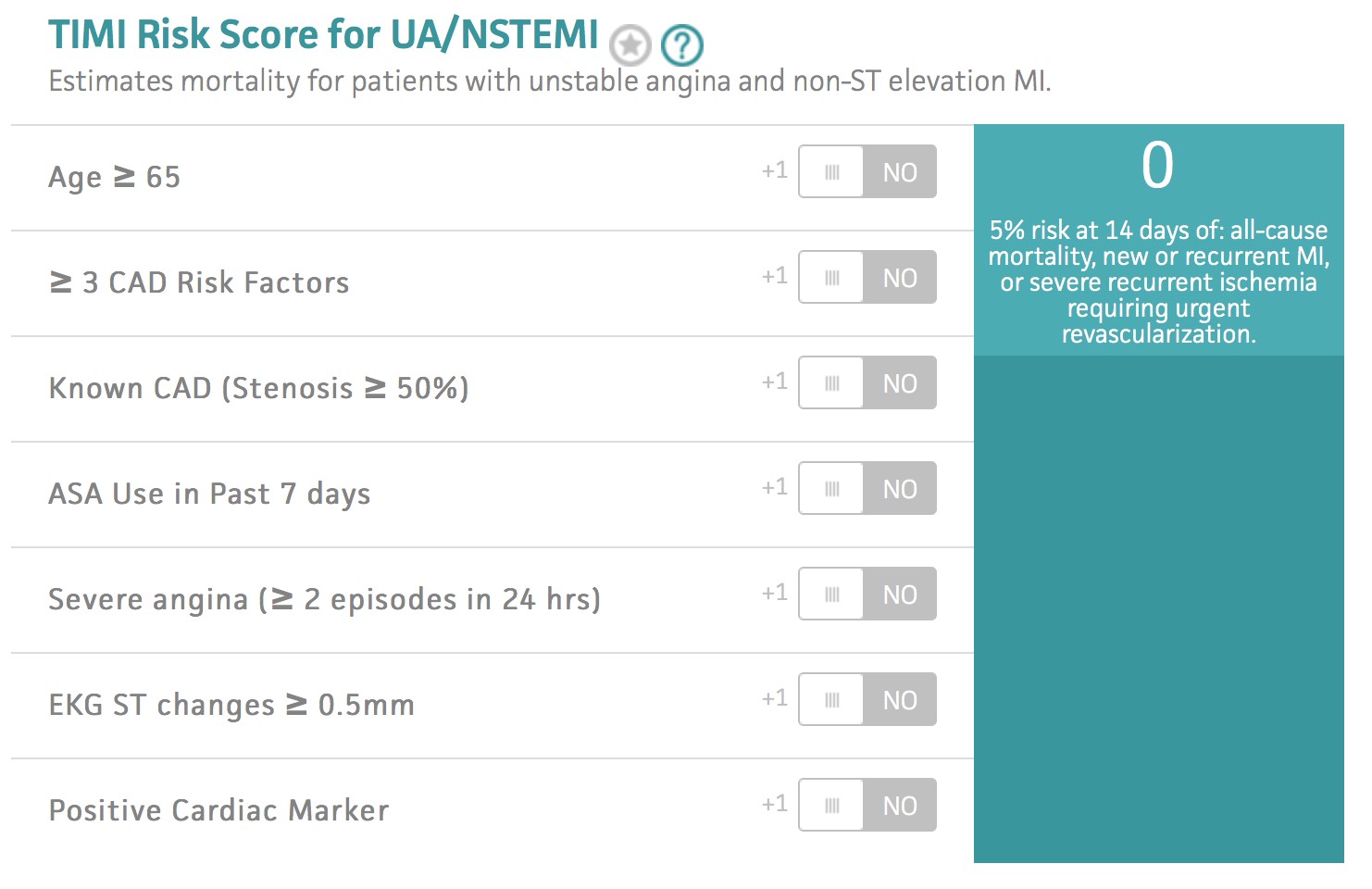
An analysis of refitted multivariate models demonstrated a marked improvement in the discriminative power of the TIMI UA/NSTEMI model with the incorporation of heart failure and hemodynamic variables. There were 137 in-hospital deaths (4%), and among the survivors, 234 (7.4%) died by 6 months post-discharge. The predictive abilities of the TIMI and GRACE scores for in-hospital and 6-month mortality were assessed by calibration and discrimination. ACS patients admitted to the University of Michigan between 19 were divided into UA/NSTEMI (n = 2753) and STEMI (n = 698) subpopulations. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
